Legislation was signed in April 2022 with the support of the MSMS-initiated and led Health Can’t Wait, a coalition with more than 50 healthcare, clinician, and patient advocacy organizations. This legislation puts more control back in the hands of clinicians and patients.
Public Act 60 of 2022 provides prior authorization (PA) reform with the goal of a quicker, more effective, and more transparent process. It does not repeal PA.
All provisions are fully in effect as of June 1, 2023, including major components such as electronic submission and faster timelines.
These reforms apply to health care insurers (and their contracted third-party vendors) and healthcare professionals whose beneficiaries/patients have commercial insurance policies regulated by the Michigan Department of Insurance and Financial Services. They do not impact Medicaid, Medicare, Medicare Advantage, or self-funded plans.
Check insurers’ provider news, updates, portals, etc. to learn of any new processes related to online submission, appeals, eligibility, and PA requirements related to the law’s implementation.
Please review the key provisions below for additional details and requirements.
Electronic Submission
Beginning June 1, 2023:
- Insurers must provide an online method through which practitioners can electronically submit PA requests for any benefits requiring PA, including prescription drugs. Facsimiles do not count as an acceptable method.
- Physicians and other health care professionals must submit PA requests electronically. The only exception is for a temporary technological or electrical failure. (NOTE: Payers have reported that access to their electronic authorization forms is available through the provider portals you use to verify eligibility and benefits.)
Timeliness of Decisions
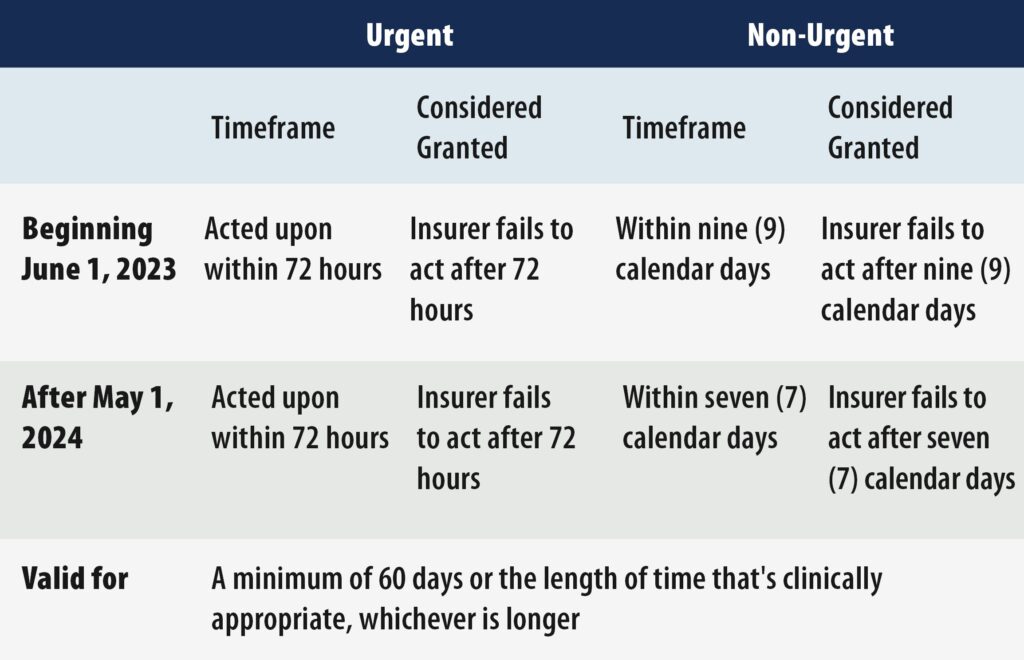
Review by Peers
Puts conditions on health care practitioners reviewing appeals (e.g., no financial stake in decision, not involved in prior denial, etc.). Any adverse determinations regarding a PA request for a non-pharmacy benefit must be made by a licensed physician and by a physician or pharmacist for a pharmacy benefit. If a denial is appealed, the denial cannot be affirmed unless it has been reviewed by a licensed physician who is board-certified or eligible in the same specialty as the service provided. An exception is allowed if finding such an individual would delay a decision within the required timeframe. In this instance, a physician in a similar general specialty could be utilized.
Clinical Validity
PA requirements must be based on peer-reviewed clinical review criteria. The criteria must:
- Take into account the needs of atypical patient populations and diagnoses.
- Reflect community standards of care.
- Ensure quality of care and access to needed health care services.
- Be evidence-based criteria.
- Be publicly available free of charge.
- Be sufficiently flexible to allow deviations from norms when justified on a case-by-case basis.
- Be evaluated and updated, if necessary, at least annually.
Transparency
PA requirements, including amendments, must be publicly and conspicuously posted online within a specified timeline. Insurers are also required to submit an annual report to the Michigan Department of Insurance and Financial Services (DIFS) which must include aggregated trend data related to the insurer’s PA practices and experience for the prior plan year. DIFS shall post an annual report with aggregated data by October 1 of each year.
In cases of PA denials, the requesting healthcare professional must be notified of the reasons for the denial and related evidence-based criteria, their right to appeal, instructions on how to file the appeal, and any other documentation necessary to support the appeal.
Gold Carding
Insurers are required to adopt a program that promotes the modification of certain PA requirements based on healthcare professionals’ adherence to nationally recognized evidence-based medical guidelines and other quality guidelines.











